 The maternal habitus can play a part in this and the role of the intrauterine pressure catheter, though effective, is not well defined.įigure 2 shows such an example, where a primigravid woman at 39+6 weeks gestation was being augmented with Syntocinon for slow progress. Clinicians typically work hard to ensure a high-quality fetal heart rate pattern is well recorded, but this is not always the case with uterine contractions. Too often the ‘unknown aetiology’ of a bradycardia is simply poorly recorded uterine hyperstimulation. Planning ahead is key in these circumstances. This is particularly important where there might be a delay in opening an operating theatre, such as in a smaller hospital out-of-hours. In recognition that some bradycardias are of unknown aetiology, reasonably, preparation for an operative delivery should form part of the overall management strategy in these cases. 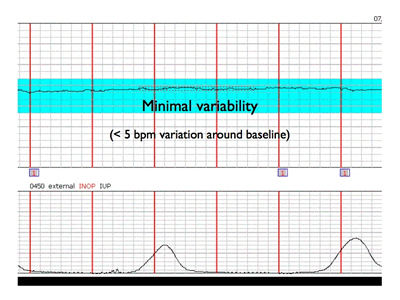
Less common causes may be placental abruption, placental infarction, uterine rupture or maternal hypoxia.įortunately, most fetal bradycardias do have a straightforward cause and are amenable to appropriate management without an emergency caesarean birth. The more common causes of sustained fetal hypoxia and subsequent bradycardia include uterine hyperstimulation (by tachysystole or hypertonus), 4 maternal hypotension (positional, procedural or anaesthetic), 5 sustained umbilical cord compression, including cord prolapse, or a rapid descent of the fetal head through the pelvis. Where the physiological basis of the fetal bradycardia is uncertain, consideration should be given to a sentinel event such as an abruption or uterine rupture. A vaginal examination should be performed to assess progress, exclude a cord prolapse, facilitate the application of a fetal scalp electrode and determine the possible mode of birth. More specific management, including delivery, will largely be determined by the overall clinical picture, an assessment of the physiological basis of the bradycardia and the response to first-line management. eliminate the uterine activity, if present, with 250μg SC terbutaline (or equivalent).correct the maternal blood pressure as required and.reposition the mother to limit cord compression and improve her blood pressure,.First-line management therefore, and to some extent regardless of the cause of the hypoxia, should be: 3 If a fetus is truly compromised, it is under perfused with oxygen. Research is clear that the longer the bradycardia, the worse the outcomes. The hypoxic fetal bradycardia is a time-critical heart rate pattern requiring immediate recognition and appropriate management. In the absence of maternal medication, the baseline bradycardia is most likely the result of a mature parasympathetic nervous system. However, it is an abnormal CTG by definition. With a baseline fetal heart rate of 90–95bpm, normal baseline variability and accelerations, this is a well-oxygenated fetus. The antenatal cardiotocography (CTG) in Figure 1 was recorded from a primigravid woman at 41+4 weeks gestation. While a fetal heart block or the accidental monitoring of the maternal heart rate may ultimately have consequences for fetal wellbeing they are not the focus of this article. 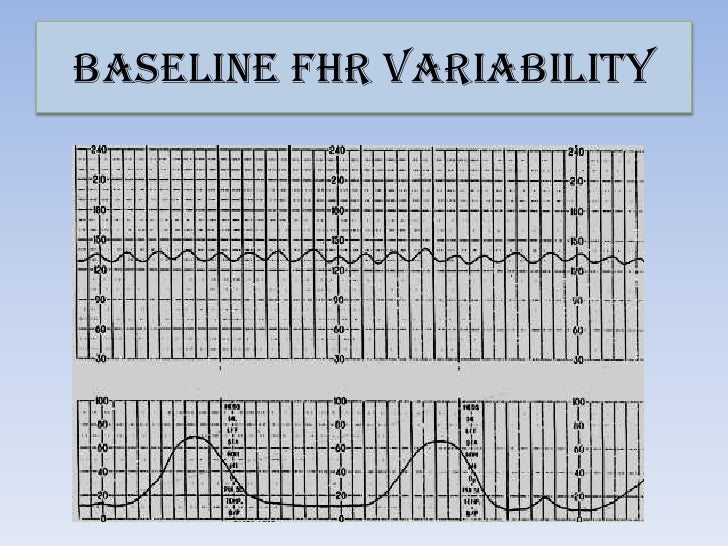
These fetuses, and indeed the mother, will generally display one or more physiologically reassuring features, such as regular movement, normal baseline variability, accelerations or even simple decelerations. The more common causes of a (non-hypoxic) fetal baseline bradycardia would include a mature parasympathetic system (Figure 1), maternal medication (high-dose beta blockers), a fetal cardiac conduction defect (heart block), or, occasionally, what turns out to be the accidental monitoring of the maternal heart rate, particularly in active labour. Given the RANZCOG IFS Guideline defines the normal baseline fetal heart rate at 110–160bpm, this would also include the fetus with a baseline fetal heart rate between 100 and 110bpm. In other words, a fetus with a bradycardia not attributable to hypoxia. In the RANZCOG Fetal Surveillance Education Program 2 (FSEP) we refer to the non-hypoxic fetal bradycardia as a baseline bradycardia. In a practical sense, however, a fetal bradycardia may be usefully thought of as being either hypoxic or non-hypoxic in origin. This is a simple definition and one which is reasonably consistent in the literature. By RANZCOG Intrapartum Fetal Surveillance (IFS) Guideline 2014 1 definition, a fetal bradycardia is a fetal heart rate (FHR) below 100 beats per minute (bpm) for more than five minutes. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
